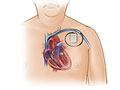
Implantable Cardioverter-Defibrillator (ICD)
Topic Overview
An implantable cardioverter-defibrillator (ICD) is a battery-powered device that can fix an abnormal heart rate or rhythm and prevent sudden death. The ICD is placed under the skin of the chest. It's attached to one or two wires (called leads). Most of the time, these leads go into the heart through a vein.
An ICD is also known as an automatic implantable cardioverter-defibrillator (AICD).
Who needs an ICD?
You might need an ICD if you have had a serious episode of an abnormally fast heart rhythm or are at high risk for having one. If you have coronary artery disease, heart failure, or a problem with the structure or electrical system of the heart, you may be at risk for an abnormal heart rhythm.
An example of a life-threatening heart rhythm is ventricular tachycardia.
- Heart Failure: Should I Get an Implantable Cardioverter-Defibrillator (ICD)?
- Heart Problems: Should I Get an Implantable Cardioverter-Defibrillator (ICD)?
How does an ICD work?
An ICD is always checking your heart rate and rhythm. If the ICD detects a life-threatening rapid heart rhythm, it tries to slow the rhythm back to normal using electrical pulses. If the dangerous rhythm does not stop, the ICD sends an electric shock to the heart to restore a normal rhythm. The device then goes back to its watchful mode.
Some ICDs also can fix a heart rate that is too slow. The ICD does so without using a shock. It can send out electrical pulses to speed up a heart rate that is too slow.
Whether you get pulses or a shock depends on the type of problem that you have and how the doctor programs the ICD for you.
How is an ICD placed?
Your doctor will put the ICD in your chest during minor surgery. You will not have open-chest surgery. You probably will have local anesthesia. This means that you will be awake but feel no pain. You also will likely have medicine to make you feel relaxed and sleepy.
Your doctor makes a small cut (incision) in your upper chest. Most of the time, he or she puts one or two leads (wires) in a vein and threads them to the heart. Sometimes, the leads are placed under the skin of your chest. Then your doctor connects the leads to the ICD. Your doctor puts the ICD under the skin of your chest and closes the incision. Your doctor also programs the ICD.
In some cases, the doctor may be able to put the ICD in another place in the chest so that you don't have a scar on your upper chest. This would allow you to wear clothing with a lower neckline and still keep the scar covered.
Most people spend the night in the hospital, just to make sure that the device is working and that there are no problems from the surgery.
You may be able to see a little bump under the skin where the ICD is placed.
How does it feel to get a shock from an ICD?
The shock from an ICD hurts briefly. It's been described as feeling like a punch in the chest. But the shock is a sign that the ICD is doing its job to keep your heart beating. You won't feel any pain if the ICD uses electrical pulses to fix a heart rate that is too fast or too slow.
There's no way to know how often a shock might occur. It might never happen.
It's possible that the ICD could shock your heart when it shouldn't. You also might be afraid or worried about when the ICD might shock you again. But you can take simple steps to feel better about having an ICD. These include having your ICD checked regularly by your doctor and making an action plan for what to do if you get shocked.
How do I live a normal, healthy life with an ICD?
You can live a normal, healthy life with your ICD. A few tips for living well with your ICD include:
- Avoid strong magnetic and electrical fields. These can keep your device from working right. Most office equipment and home appliances are safe to use. Learn which things you should use with caution and which you should stay away from.
- Know what to do when you get a shock from your ICD.
- Be sure that any doctor, dentist, or other health professional you see knows that you have an ICD.
- Always carry a card in your wallet that tells what kind of device you have. Wear medical alert jewelry that says you have an ICD.
- Have your ICD checked regularly to make sure it's working right.
- It's common to be anxious that the ICD might shock you. But you can take steps to think positively and worry less about living with an ICD.
Talk with your doctor about the possibility of turning off the ICD at the end of life. Many people consider turning off the ICD when their health goals change from living longer to getting the most comfort possible at the end of life. Turning off your ICD is legal. It isn't considered suicide. The decision to leave on or turn off your ICD is a medical decision that you make based on your values. You can put your wishes in an advance directive.
For more tips, see:
Health Tools
Health Tools help you make wise health decisions or take action to improve your health.
Other Places To Get Help
Organizations
Related Information
References
Other Works Consulted
- Baddour LM, et al. (2010). Update on cardiovascular implantable electronic device infections and their management. A scientific statement from the American Heart Association. Circulation, 121(3): 458-477.
- Chang PM, et al. (2014). Subcutaneous implantable cardioverter-defibrillator. Circulation, 129(23): e644-e646. DOI: 10.1161/CIRCULATIONAHA.113.006645. Accessed April 11, 2017.
- Epstein AE, et al. (2008). ACC/AHA/HRS 2008 Guidelines for Device-Based Therapy of Cardiac Rhythm Abnormalities: A Report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Writing Committee to Revise the ACC/AHA/NASPE 2002 Guideline Update for Implantation of Cardiac Pacemakers and Antiarrhythmia Devices): Developed in Collaboration With the American Association for Thoracic Surgery and Society of Thoracic Surgeons. Circulation, 117(21): e350-e408. [Correction in Circulation, 120(5): e34-e35.]
- Lampert R, et al. (2010). HRS Expert Consensus Statement on the Management of Cardiovascular Implantable Electronic Devices (CIEDs) in patients nearing end of life or requesting withdrawal of therapy. Heart Rhythm, 7(7): 1008-1026. Available online: http://www.hrsonline.org/Policy/ClinicalGuidelines/upload/ceids_mgmt_eol.pdf.
- Sears SF, et al. (2005). How to respond to an implantable cardioverter-defibrillator shock. Circulation, 111(23): e380-e382.
- Sears SF, et al. (2011). Posttraumatic stress and the implantable cardioverter-defibrillator patient. Circulation: Arrhythmia and Electrophysiology, 4(2): 242-250.
- Swerdlow CD, et al. (2015) Pacemakers and implantable cardioverter-defibrillators. In DL Mann et al., eds., Braunwald's Heart Disease: A Textbook of Cardiovascular Medicine, 10th ed., vol. 1, pp. 721-742. Philadelphia: Saunders.
- Wilkoff BL, et al. (2008). HRS/EHRA expert consensus on the monitoring of cardiovascular implantable electronic devices (CIEDS): Description of techniques, indications, personnel, frequency, and ethical considerations. Heart Rhythm, 5(6): 907-925. Available online: http://www.hrsonline.org/Practice-Guidance/Clinical-Guidelines-Documents/HRS-EHRA-Expert-Consensus-on-the-Monitoring-of-Cardiovascular-Implantable-Electronic-Devices/2008-Monitoring-of-CIEDs.
Credits
ByHealthwise Staff
Primary Medical Reviewer Rakesh K. Pai, MD, FACC - Cardiology, Electrophysiology
Martin J. Gabica, MD - Family Medicine
E. Gregory Thompson, MD - Internal Medicine
Elizabeth T. Russo, MD - Internal Medicine
Adam Husney, MD - Family Medicine
Specialist Medical Reviewer John M. Miller, MD, FACC - Cardiology, Electrophysiology
Current as ofJanuary 12, 2018
- Top of Page
Next Section:
Health Tools
Previous Section:
Topic Overview- Top of Page
Next Section:
Other Places To Get Help
Previous Section:
Health Tools- Top of Page
Next Section:
Related Information
Previous Section:
Other Places To Get Help- Top of Page
Next Section:
References
Previous Section:
Related Information- Top of Page
Next Section:
Credits
Previous Section:
References- Top of Page
Current as of: January 12, 2018
Author: Healthwise Staff
Medical Review: Rakesh K. Pai, MD, FACC - Cardiology, Electrophysiology & Martin J. Gabica, MD - Family Medicine & E. Gregory Thompson, MD - Internal Medicine & Elizabeth T. Russo, MD - Internal Medicine & Adam Husney, MD - Family Medicine & John M. Miller, MD, FACC - Cardiology, Electrophysiology